New research indicates that vitamin D supplementation may alter the way the immune system interacts with gut bacteria in patients with inflammatory bowel disease (IBD), potentially shifting the body towards a more balanced and less inflamed state. This discovery suggests a new avenue for therapies that focus on restoring immune tolerance, rather than just suppressing symptoms.
Understanding Inflammatory Bowel Disease
IBD, encompassing conditions like ulcerative colitis and Crohn’s disease, is a chronic inflammatory disorder of the digestive tract. It arises from a complex combination of genetic predisposition and environmental triggers. A key factor in its development is the loss of immune tolerance to the trillions of bacteria naturally residing in the gut. Current treatments primarily target the symptoms of inflammation, but don’t address the root cause: the miscommunication between the immune system and gut microbiome.
How Vitamin D May Help
The study, conducted by researchers at Mayo Clinic, evaluated 48 IBD patients with low vitamin D levels. Participants received weekly supplements for 12 weeks, and researchers analyzed blood and stool samples to map how the immune system responded to gut bacteria before and after treatment.
Key findings include:
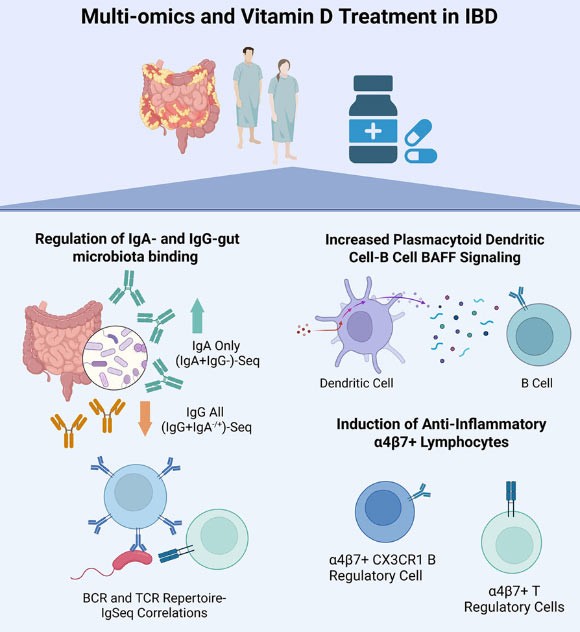
- Increased IgA levels: Vitamin D supplementation was linked to higher levels of immunoglobulin A (IgA), an antibody typically associated with protective immune responses.
- Decreased IgG levels: Simultaneously, levels of immunoglobulin G (IgG) – often linked to inflammation – were reduced.
- Shift in Immune Signaling: The study also observed changes in immune signaling pathways, with increased activity in regulatory immune cells, which help control inflammation.
- Improved Disease Markers: Participants showed improvements in disease activity scores and reduced inflammation in stool samples.
“This study suggests vitamin D may help rebalance how the immune system sees gut bacteria,” explained Dr. John Mark Gubatan, a gastroenterologist at Mayo Clinic. “That’s an important step toward understanding how we might restore immune tolerance in IBD.”
Caution and Future Research
While these results are promising, researchers emphasize the study’s limitations. The sample size was small, and the design was not a randomized controlled trial, meaning it cannot definitively prove cause and effect. Larger, more rigorous studies are needed to confirm these findings.
Dr. Gubatan cautioned against self-treating with vitamin D, stressing that dosage should be individualized under medical supervision, especially in patients with chronic inflammation.
The study was published in the journal Cell Reports Medicine (doi: 10.1016/j.xcrm.2026.102703).
These findings suggest that vitamin D may play a critical role in modulating immune-microbiome interactions, but more research is essential to translate these insights into effective therapies for IBD.